A systematic understanding of the effects of pain on the different body systems helps to choose the most effective pain management strategies.
The body’s adaptive response to pain involves physiological changes, which are useful and potentially life-saving in the initial stages. If the adaptive response persists, harmful and life- threatening effects may ensue. Pain is noxious, which makes it a powerful protective force: indeed, the inability to feel pain is associated with a shortened life expectancy.
Pain has much in common with other sensory modalities (National Academy of Sciences, 1985). First, there are specific pain receptors. These are nerve endings, present in most body tissues, that only respond to damaging or potentially damaging stimuli. Second, the messages initiated by these noxious stimuli are transmitted by specific, identified nerves to the spinal cord. The sensitive nerve ending in the tissue and the nerve attached to it together form a unit called the primary afferent nociceptor. The primary afferent nociceptor contacts second-order pain- transmission neurons in the spinal cord.
The second-order cells relay the message through well-defined pathways to higher centers, including the brain stem reticular formation, thalamus, somatosensory cortex, and limbic system.
It is thought that the processes underlying pain perception involve primarily the thalamus and cortex. Pain is the body’s way of telling you something is wrong, and can be beneficial, raising your awareness of danger. Acute pain, such as the burn from a hot surface, tells your brain to move your hand away quickly.
Chronic pain, as the term implies, is long-lasting; there’s no universally agreed-upon definition, but most doctors consider pain lasting several months to be chronic. Arthritis, nerve damage and diseases such as multiple sclerosis are common causes of chronic pain. Nearly 50 million American adults experience chronic pain, according to statistics compiled by the Centers for Disease Control and Prevention.
Emotions and the Chronic Pain Cycle
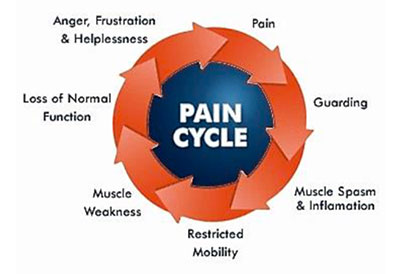
Pain is also influenced by emotions, and the cycle of pain and emotions are interrelated. Emotions may directly impact physical change as well. For example, when you are anxious or angry, your muscles may tighten, and that physical change may also contribute to increased pain.
Another challenge may be that patients might feel stigmatized when they demonstrate intense emotions like these in the context of their treatment.
Believing that you have control over your life and can
continue to function despite the pain or subsequent life changes has been shown to decrease depression.
Cannabinoid Receptors
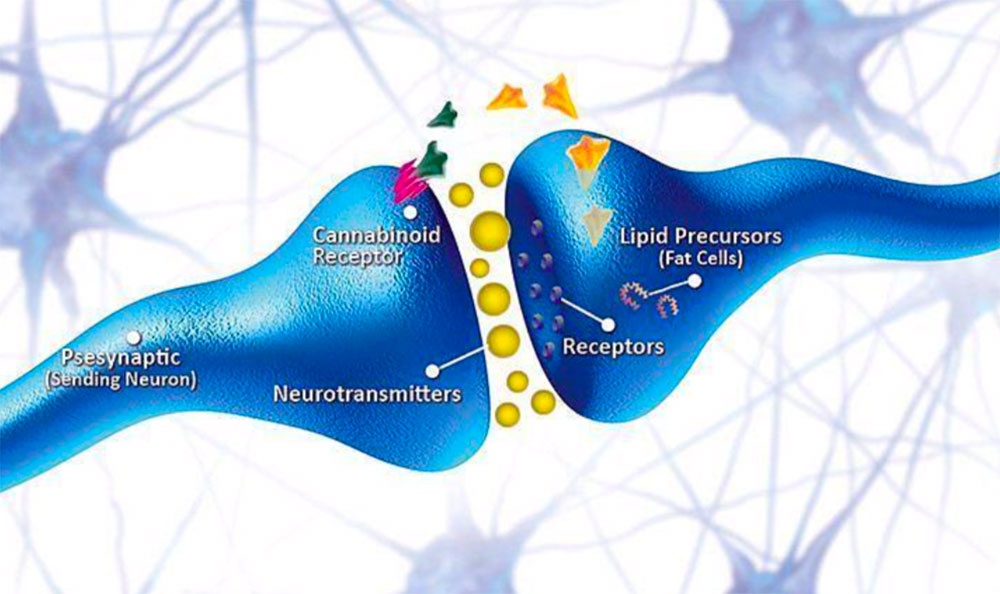
Cannabinoid receptors are currently classified into three groups: central (CB1), peripheral (CB2) and GPR55, all of which are G-protein- coupled. CB1 receptors are primarily located at central and peripheral nerve terminals. CB2 receptors are predominantly expressed in non-neuronal tissues, particularly immune cells, where they modulate cytokine release and cell migration.
Recent reports have suggested that CB2 receptors may also be expressed in the CNS. GPR55 receptors are non-CB1/CB2 receptors that exhibit affinity for endogenous, plant and synthetic cannabinoids. Endogenous ligands for cannabinoid receptors have been discovered, including anandamide and 2-arachidonylglycerol.
Managed improperly, chronic pain can become a debilitating condition that impacts all areas of a patient’s life, from sleep and mental health to cognitive processes and cardiovascular health. Chronic pain can be extremely difficult to treat and one of the reasons why scientists have trouble finding the best treatment pathways is because the complicated nature of pain isn’t yet fully understood. For many years, opioids have been the go-to solution for patients dealing with chronic pain, but, according to National Institute on Drug Abuse, nearly 30% of patients who are prescribed opioids misuse them and up to 12% develop an addiction.
According to biotechnology industry executive Alan Dunton, one of the biggest challenges in developing pain treatments is the incomplete assessment of pain, and this is where innovations should begin.
The aged “pain chart” that most physicians still rely on today isn’t always helpful, because pain is subjective and patients can’t always explain where the pain is localized and how much it hurts. But combined with the Electronic Patient Visit Assessment system developed by Janet Van Cleave, it could become more accurate. Although bias is still a risk, AI-powered biomarker should help doctors analyze the pain data of patients and add more objectivity in the assessment process.
The results from using the AB Centric’s Pain & Inflammation patch has been significant in a recent study. Fourth eight out of fifty clients received an 85% reduction in pain and inflammation. This study was conducted from a chronic persistent inflammation that was caused from many diseases including Alzheimer’s, arthritis, asthma, colitis, irritable bowel syndrome and multiple sclerosis.
There are 5 main symptoms of inflammation that are characterized by the Latin words dolor (pain), redness, tumor (swelling), heat and (loss of function). Inflammatory diseases are often associated with perturbations to the immune system and an automatic immune response with some exceptions including atherosclerosis. You may want to run and hide from chronic pain. But pain, it seems, does its best to hide from medication taken to provide relief.
An international team of researchers has found that chronic pain can be hard to treat because pain receptors normally found on nerve cell surfaces can move, migrating into the cell, which places them out of the reach of pain medications while they continue to pump out pain signals to the brain.
Luckily, new lines of research show that the future of pain management may not lie in prescribing more pills. The latest innovations in pain treatment now give patients more choices and early results of experimental technologies could reduce the need for painkillers to a minimum.
Our Solution
- Pain & Inflammation – (Addresses inflammation in the body that causes most pain syndromes).
- Fibromyalgia – (Designed to address pain associated with Fibromyalgia).
- Migraine – (Assists in reducing migraine headaches that can cause intense throbbing).
- Nerve Stimulation – (Promotes the healing process of nerve damage and bone support).
- Ultra Joint Plus– (Addresses joint specific issues and relieves discomfort).
Our technology is made as a complementary method of achieving behavioral responses. We are not in competition with standard medical practice or a medical procedure that uses traditional therapy. We make products that work on a different part on the body that triggers responses through electrical pathways to prevent disorders.





